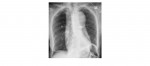
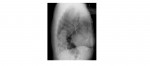
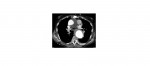
The following chest x-rays are from a 70 year old with severe chest and interscapular back pain. What can you conclude from the x-rays?
[peekaboo_link name=”Answer”]Answer[/peekaboo_link] [peekaboo_content name=”Answer”]
The frontal chest x-ray shows a widening of the mediastinum. The most useful out of the two views is the lateral chest radiograph which clearly shows the thoracic aortic dilatation involving the ascending arch and the descending thoracic aorta. A prosthetic aortic valve is present and there are also sternal wires.
The clinical symptoms in combination with the x-ray features should raise suspicion for a thoracic aortic dissection.
Contrast enhanced CT chest showed aneurysmal dilatation of the aortic root, ascending, arch and the descending thoracic aorta with extensive intramural haematoma and an intimal flap in the descending aorta extending proximally as well as distally. The CT features were in keeping with a Stanford type A aortic dissection.
Preferred imaging examination for aortic dissection is contrast enhanced CT of the chest. A normal chest x-ray does not rule out an aortic dissection.
What are the chest x-ray findings of a thoracic aortic dissection?
- Mediastinal widening is the most common finding (found in approximately 80% of cases).
- Double aortic knob sign.
- Diffuse enlargement of the aorta with poor definition of the aortic contour.
- Calcium sign: inward displacement of the aortic wall calcification by more than 10mm.
- Tracheal displacement to the right.
- Pleural effusion (more common on the left side).
- Pericardial effusion.
- Displacement of the nasogastric tube.
- Left apical opacity.
Reference: http://emedicine.medscape.com/article/416776-overview#a19
[/peekaboo_content]